Introduction:
Endoscopic third ventriculostomy (ETV) is a neuorsurgical procedure performed for obstructive hydrocephalus where a near physiologic CSF circulation is restored by making a permanent defect in the floor of the third ventricle anterior to the mammillary bodies,
thus connecting it to the interpeduncular.
The overall complication rates reported in published series varies widely from 4–30%,
but the overall rate of serious complications is less than 10% including an infection rate of 3%,
and hemorrhage rate 2.5%.
Late failure occurs in up to 40%.
Anatomical Patency:
Radiological outcomes alone may be misleading.
After a successful ETV,
the size of the ventricular system can require a few months to stabilize.
To evaluate patency,
helpful signs include: demonstration of mid-sagittal surgical defect of the floor of the third ventricle,
and resolution of hydrocephalus and periventricular edema.

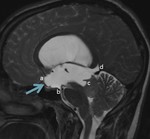
Fig. 1: Anatomy of the third ventricle as seen on 2D turbo spin echo T2WI:
The lamina terminalis (a), third ventricular floor (b), aqueduct (proximal portion is enlarged in this case) (c), and suprapineal recess overlays the pineal gland inferiorly (d). Note the suprachiasmatic recess bowing (Bowing sign) on this preoperative MRI (blue arrow).
A- The Ostomy:
Midline sagittal T2 weighted and sagittal constructive interference in steady state (CISS) high resolution MRI images is useful in the post-operative evaluation of the patency of the created ostomy.
A small percentage will close in the first year of follow up,
but the vast majority will show increase in the size of the ETV defect.

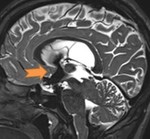
Fig. 2: T1 (left) and 3D CISS sequence (right) in the sagittal plane demonstrating anatomical patency of the ventriculostomy site in the floor of the third ventricle. Note the tectal glioma in this case.
- A change in ventricular size is less important after third ventriculostomy.
- Volumetric measurements calculated from standard CT scans will show a demonstrable decrease in ventricular volume soon after successful third ventriculostomy.
Third ventricle may show a 33% reduction in the in patients whose symptoms have been successfully controlled.
Lateral ventricles will only decrease by 16% in size on average.
- Although the third ventricle may exhibit a greater decrease,
the lateral ventricular measurements are more accurate.
Patients with more indolent symptoms show the smallest change.
- Enlargement of the size of the ventricles as demonstrated on follow up CT may indicate failure
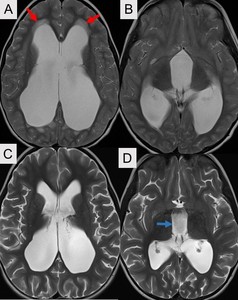
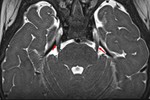
Fig. 3: T2 weighted axial MRI images. Panels (A and B) are pre-operative and show moderate to severe triventricular upstream hydrocephalus with transependymal flow (red arrows). Post operative MRI (Panels C and D) show interval decrease in prominence of the third and lateral ventricles. Note the flow voids in third ventricle (blue arrow) related to flow through the ostomy. The tranependymal flow has resolved.
Functional Patency:
Besides the anatomical information that can be obtained with multiplanar high spatial and contrast resolution imaging,
functional information and analysis of CSF flow dynamics can also be clinically relevant.
The presence of a flow void appears to correlate with clinical success,
and the absence of flow void correlates with clinical failure.
Various motion sensitive MRI techniques can be used in the evaluation of CSF flow (3D SPACE,
3D CISS and cine phase contrast).

Fig. 4: 3D SPACE sequence in the sagittal demonstrating prominent flow artifact at the site of the ETV as high velocity signal loss suggestive of anatomical and functional patency.
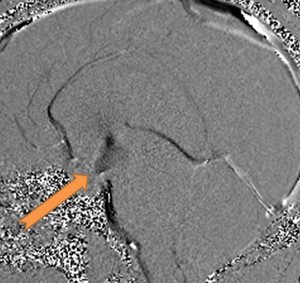
Fig. 5: phase contrast sequence in the sagittal plane demonstrating functional flow through the site of the ETV.

Fig. 6: Cine phase contrast sequence in the sagittal plane demonstrating functional flow through the site of the ETV. Downward flow through the ostomy site is white, the pulsation flow in the basilar artery is black.

Fig. 7: Cine phase contrast sequence in the sagittal plane demonstrating functional flow through the site of the ETV.

Fig. 8: Cine phase contrast sequence in the axial plane demonstrating functional flow through the site of the ETV. Downward flow through the ostomy site is white, the pulsation flow in the basilar artery is black.

Fig. 9: Visual comparison of flow as detected on the CISS (left), SPACE (middle), and phase contrast (right) sequences in the same patient.
Other complications:
Complications of ETV include: intraventricular hemorrhage,
subdural hematoma intracerebral hemorrhage,
subdural hygroma,
damage to the fornices and hypothalamus,
vascular injury,
cranial neuropathy,
Hypertrophic calcifications,
and infection (ventriculitis/ meningitis).
Subdural Hygroma:
- The CSF forces its way through the frontal tract and into the subdural space because the newly created pathways and the absorptive mechanisms need time to mature.
- Crescentic CSF density/signal accumulation of CSF in subdural space that does not extend into the sulci.

Fig. 10: Three different patients with right (A), left (B), and bilateral (C) subdural hygromas post ETV demonstrated on T2 axial MRI.
Infection:
- Postoperative meningitis/ventriculitis present with fever,
headache,
vomiting,
and signs of intracranial hyper tension within 2-7 days.

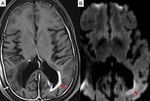
Fig. 11: Post contrast T1 axial MRI (A) showing diffuse meningeal enhancement (yellow arrow) which can bee seen with meningitis. There is also evidence of ventriculitis (red arrows) including ependymal enhancement (A) and diffusion restriction (B) in the left occipital and atrial region of the lateral ventricle.
Intracerebral / Intraventricular Hemorrhage:
- Related to the passage of the endoscopic instruments with confounding factor of decreased ventricular size and release of pressure.
- Most hemorrhages are asymptomatic.
- Intracerebral hemorrhage typically occurs in a relatively non-eloquent area.

Fig. 12: Post ETV evaluation of three different patients. The first (A) is axial non enhanced axial CT showing right intraventricular hemorrhage (red arrow) and left penumocephalus (blue arrow). Second (B) T2 axial MRI showing right penumoventricle (yellow arrow) and small bilateral intraventricular hemorrhage. (C) axial GRE demonstrate blooming of the brain parenchyma about the lateral ventricles bilaterally, consistent with blood products.
Subdural Hematoma:
- Usually small and asymptomatic,
but occasionally massive with serious outcome.
- Excessive loss of CSF can lead to unilateral,
contralateral,
or bilateral acute or chronic subdural hematomata

Fig. 14: Right subdural hematoma post ETV seen on T2 axial MRI.
Forniceal injury:
- Likely the most common complication of ETV.
- Can lead to memory disturbances,
but usually of minimal or negligible clinical consequences.
- Usually unilateral,
however contralateral and bilateral injuries have been reported.
- May show on CT as unilateral (or bilateral) forniceal hemorrhage.
- On MRI: initially,
the injured fornix may be swollen with hyperintensity on T2 weighted images.
The forniceal bodies may also restrict on Diffusion weighted images (DWI).
Later,
reduction in volume in addition to atrophy elsewhere like in corpus callosum and hippocampi can occur.
Anisotropy measures and tractography may demonstrate disruption of the forniceal fibers.

Fig. 15: Panel A and B show normal appearance of the fornix on Coronal T2 WI and Sagittal T1WI respectively. Panel C show chronic fonriceal atrophy as well as atrophy of the corpus callosum. Note the ETV site.
Basilar Artery Injury:
- Damage to the basilar artery or its branches is the most life-threatening complication and is related to perforating the floor of the third ventricle.
- More common than damage to the basilar bifurcation is damage to its perforators.
- An angiogram should be arranged when the patient becomes neurologically stable,
and if a traumatic aneurysm.
- On CT and MRI evaluate for hemorrhage,
related stroke or pseudoaneurysm formation.
Cranial Neuropathies:
- Rare complications,
occurs due to stretch of the floor.
- Oculomotor and the abducens are the most affected.
- The oculomotor nerve root emerges into the interpeduncular cistern,
and this root entry zone in the cistern.
- The abducens courses anteriorly through the pons to the pontomedullary junction and into the prepontine cistern.
- Steady-state free precession (SSFP) sequences can provide a high spatial resolution for evaluation of cranial nerves.

Fig. 16: SSFP MR image at the level of the pontomedullary junction shows normal appearing right abducens nerve as it enters the Dorello canal.

Fig. 17: SSFP MR image showing normal appearance of the bilateral trigeminal nerves
Hypertrophic calcification:
- These have been reported in the literature.
It ispostulated that this complication is iatrogenic from sealing the burr hole with bone dust at the conclusion of the procedure.
It may have been from the scope carrying bone dust through the cerebrum.